What are the Symptoms of Psoriasis?
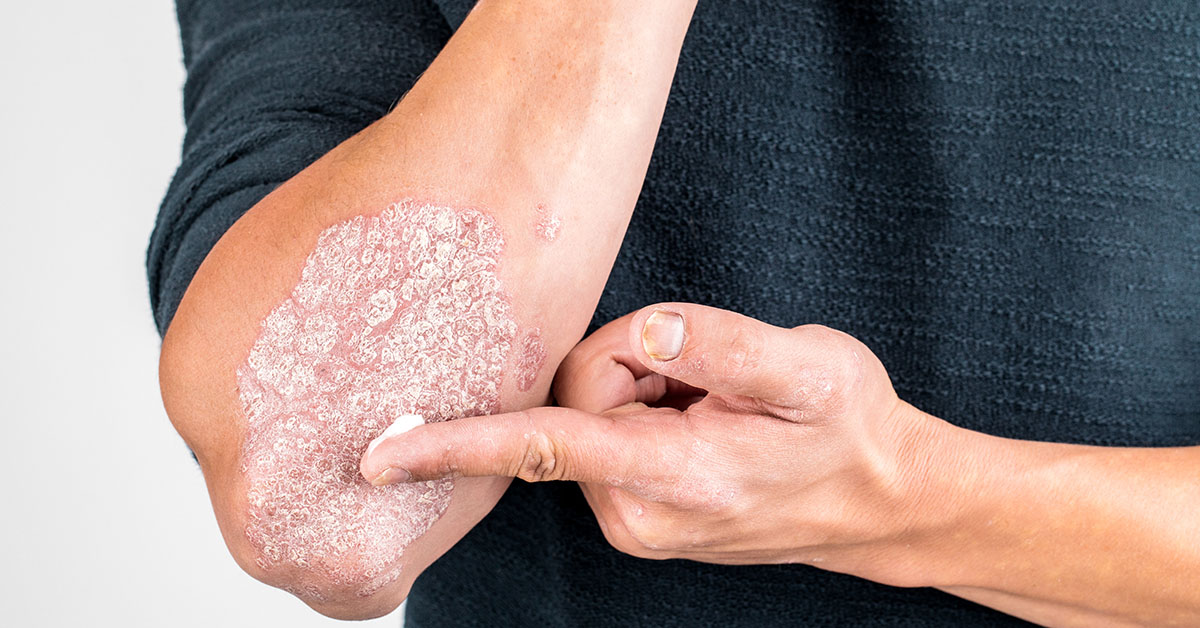
Psoriasis is a skin condition that causes red, scaly, itchy patches mainly found around the knees, trunk, elbows, and scalp. It is a painful chronic illness that primarily evolves over phases with occasional flareups lasting weeks or months and sudden subsiding periods or remissions. Many dermatologists prescribe ointments to manage the symptoms and pain, while others prescribe lifestyle changes and coping behaviors to help patients live a more comfortable life.
Signs and symptoms of psoriasis
Usually, symptoms of the disease vary between patients, but most of the symptoms have similar signatures, including:
- Dry, cracked skin that may bleed or itch
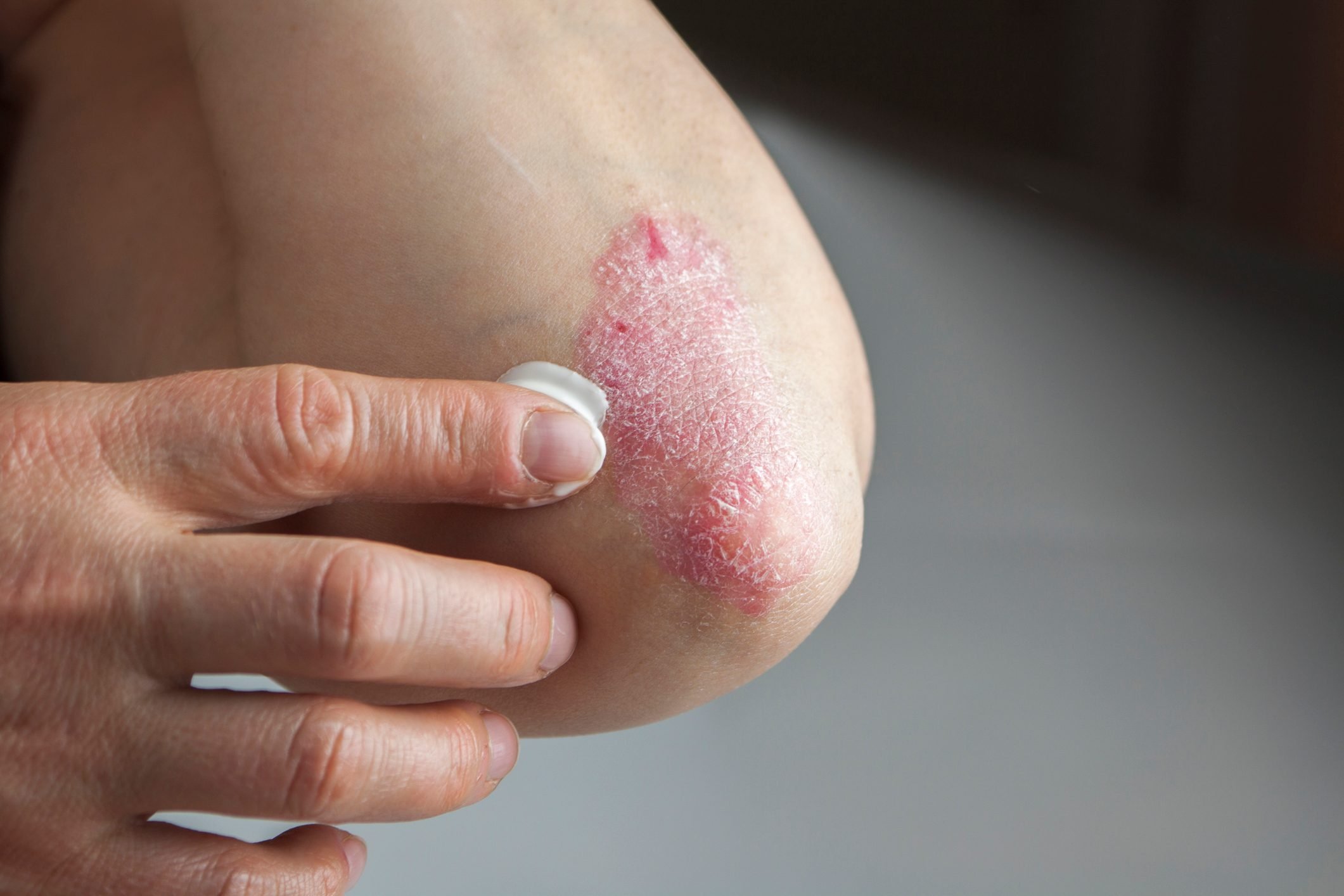
- Red patches of skin covered with thick, silvery scales
- Thickened, pitted, or ridged nails
- Small scaling spots (commonly seen in children)
- Swollen and stiff joints
- Itching, burning, or soreness
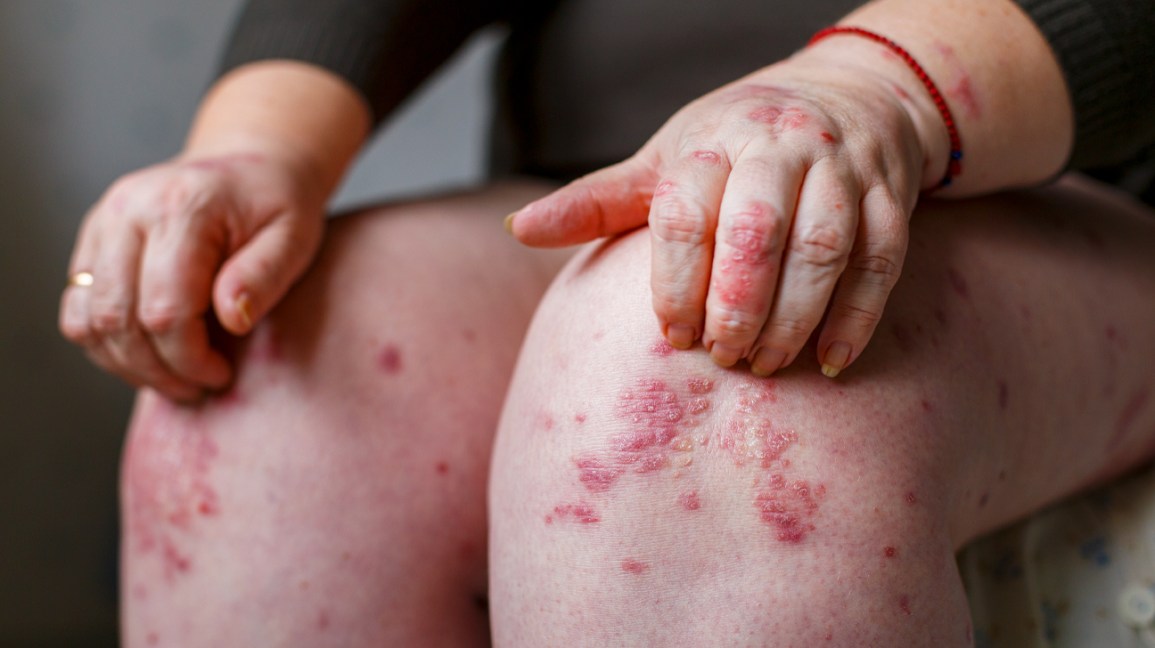
Patches caused by the disease can range from few spots on the skin resembling dandruff-like scaling to large eruptions that cover broad areas of skin. The most commonly affected body regions are the palms, scalp, knees, lower back, soles of the feet, scalp, and face.
What are the possible triggers of psoriasis?
Many predisposed patients may express virtually no symptoms for several years until the illness is triggered by an environmental factor or exposure to certain environments or conditions.
Common psoriasis triggers
- Cold or dry weather conditions outside the patient’s norm.
- Infections, such as strep throat infections.
- Skin injury, such as a scrape or cut, severe sunburn, or a bug bite.
- Heavy alcohol consumption.
- Stress for extended periods.
- Smoking and exposure to secondary smoking.
Psoriasis treatment and management options
Several treatments and management approaches can be used depending on how patients respond to the drugs and the severity of the condition. Some of the options to consider include:
Certain medications, including high blood pressure medications, lithium, and antimalarial drugs. This approach can also include oral corticosteroids. Also, you could use beta-blocker drugs used in the management of heart disease and high blood pressure.
Exposure to cold, dry weather
Any climate that relieves dry skin will help alleviate your symptoms. So try to spend more time in a warm atmosphere with high humidity.
Stress management
Always try to relax and keep calm because outbreaks often occur when a patient is stressed out.
Immediately manage gateway infections
Infections like strep throat and tonsillitis should be kept at bay at all times to stop them from leading to flare-ups.
Be watchful of skin injuries
In some patients, the smallest cuts can lead to serious outbreaks. If you have been diagnosed with dormant psoriasis, you should be extra safe with any sharp object, as even a minor cut can lead to a flare-up. Try putting on gloves or wearing extra clothes for additional protection from skin damage.
Avoid alcohol consumption
Heavy drinking, especially in young men, may trigger or make psoriasis outbreaks more severe and even interfere with treatment because combining certain psoriasis drugs with alcohol has dangerous side effects.
Quit smoking
Tobacco use or exposure to secondary smoke puts patients at risk of attack or worsens outbreak symptoms. So make sure you stay away from smokers and avoid smoking too.
Using tobacco or being around second-hand smoke raises your risk of getting psoriasis and worsens existing conditions.
Final thoughts
Psoriasis treatment can be different depending on the severity of the condition, the type of skin the patient has, and the location of the outbreak. Either way, patients can be prescribed a manageable routine that will guarantee a comfortable life while suffering from psoriasis. Patients should try to follow their doctor’s instructions to ensure a speedy recovery or a reduction in symptoms over time.




